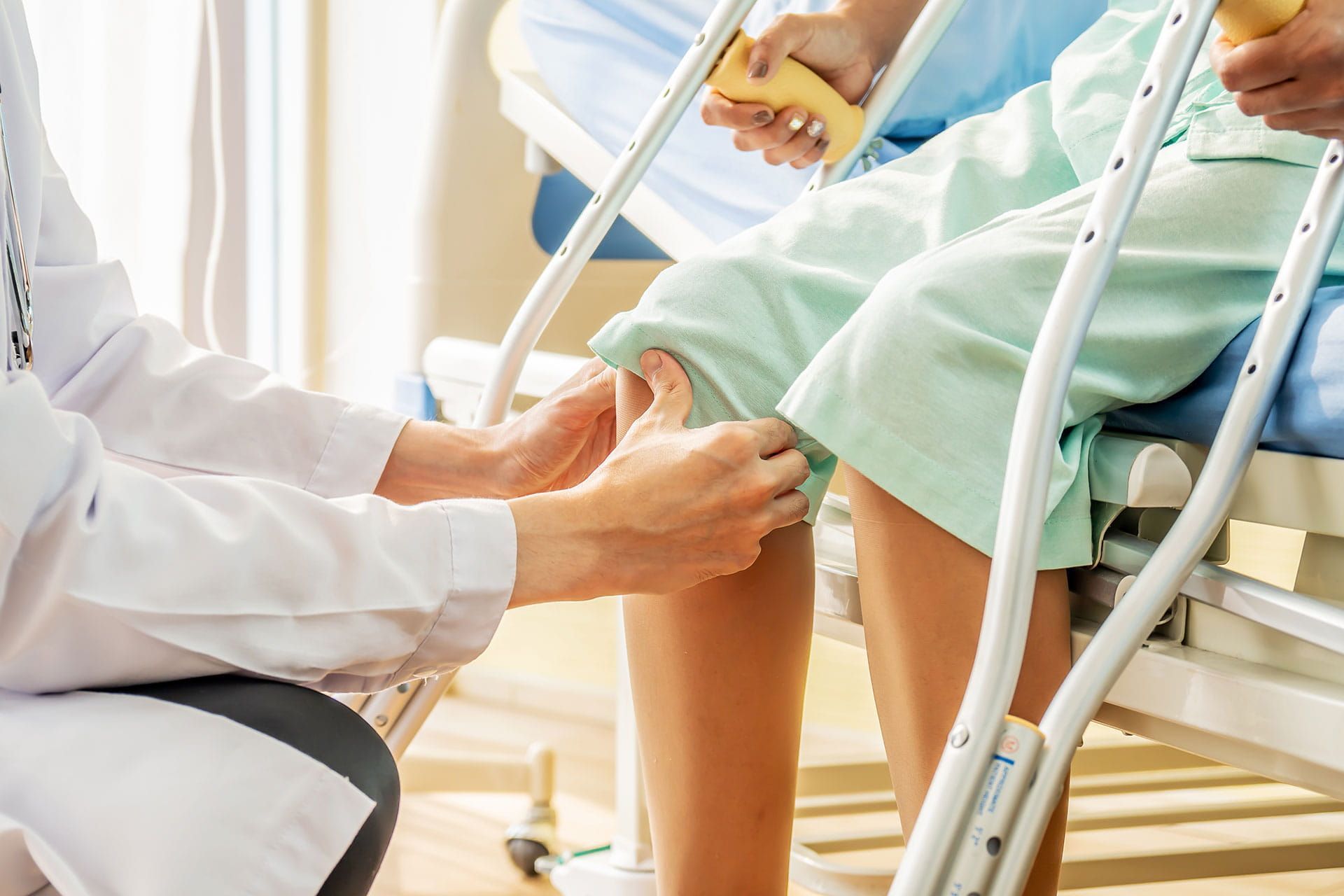
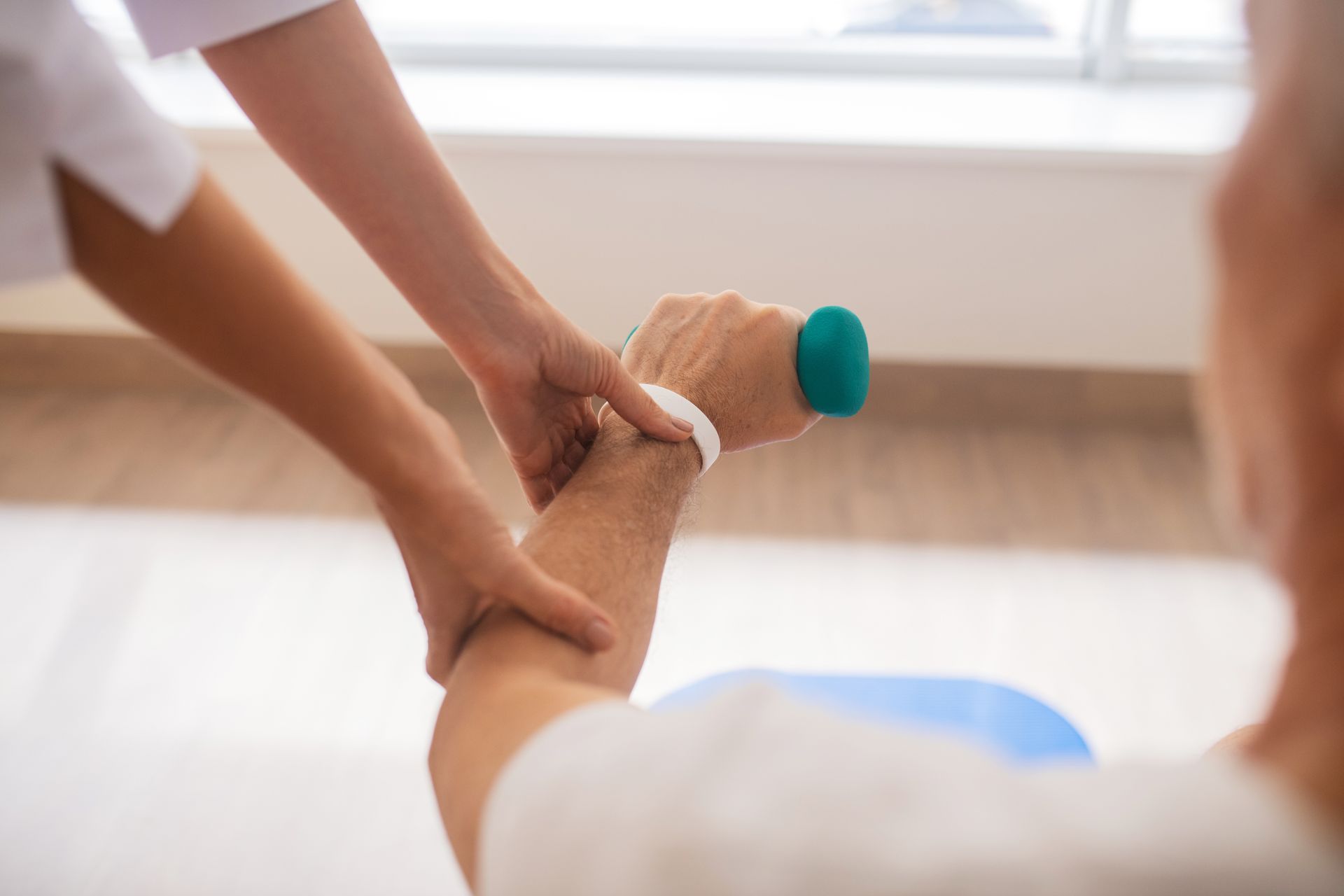
Arthritis
Arthritis doesn't have to mean the end of an active life. With the right physiotherapy approach, millions of people reclaim strength, mobility, and the everyday joys that pain had taken from them.
Arthritis affects over 350 million people globally — and yet it remains one of the most misunderstood conditions in modern healthcare. Too often, patients are told to "rest more" or simply handed a prescription, when in reality the most powerful tool for long-term arthritis management may be structured, guided movement: physiotherapy.
Whether you're living with osteoarthritis, rheumatoid arthritis, or psoriatic arthritis, physiotherapy offers a research-backed, personalized pathway to less pain, better function, and improved quality of life. This guide breaks down everything you need to know.
What Is Arthritis, Really?
Arthritis is not a single disease — it's an umbrella term for over 100 conditions that affect the joints, surrounding tissues, and connective structures. The two most common forms are osteoarthritis (OA), which involves the breakdown of cartilage, and rheumatoid arthritis (RA), an autoimmune condition causing joint inflammation. Common symptoms across both include joint stiffness (especially in the morning), swelling, tenderness, reduced range of motion, and chronic pain that fluctuates with activity and weather. Left unmanaged, arthritis can significantly limit independence and mental wellbeing.
The Role of Physiotherapy: Why Movement Is Medicine
It may seem counterintuitive — if your joints ache, shouldn't you avoid moving them? The answer, backed by decades of clinical research, is a firm no. Gentle, strategic movement nourishes cartilage, strengthens the muscles that support joints, reduces inflammation, and prevents the stiffness cycle that worsens over time with inactivity.
A qualified physiotherapist will assess your specific joints, strength imbalances, movement patterns, and pain levels to build a program that challenges your body safely and progresses over time.
Start your physiotherapy journey with a thorough assessment. A good physio doesn't just hand you a sheet of exercises — they watch how you move, identify compensatory patterns, and tailor everything to your unique presentation. What works for knee OA in one patient may be entirely wrong for another.
Physiotherapy Techniques That Work
Therapeutic Exercise
Targeted strengthening of muscles around affected joints reduces load on cartilage and improves stability. Resistance training, gentle stretching, and low-impact aerobics are cornerstones of any arthritis program.
Manual Therapy
Hands-on joint mobilisation and soft tissue massage can restore range of motion, ease stiffness, and reduce pain — particularly effective in early-to-mid stage osteoarthritis of the hip and knee.
Electrotherapy (TENS)
Transcutaneous electrical nerve stimulation (TENS) and ultrasound therapy are used to interrupt pain signals and promote tissue healing, offering drug-free pain relief between flare-ups.
Orthotics & Bracing
Custom-fitted insoles, knee braces, or splints can redistribute joint load, improve alignment, and significantly reduce pain during daily activities — particularly for knee and foot arthritis.
Postural & Gait Training
Many arthritis patients develop compensatory movement habits that stress other joints. Physiotherapists retrain movement patterns to reduce overall wear and minimise secondary injuries.
Getting Started
Exercises You Can Begin Today
While a professional assessment is always recommended before starting any program, here are physiotherapist-approved exercises suitable for most arthritis patients. Move slowly, breathe steadily, and stop if pain increases significantly.
Seated Knee Extensions: Sit in a chair, slowly straighten one leg until it's parallel to the floor. Hold 3 seconds. Lower slowly. 10 reps each side. Strengthens the quadriceps, reducing load on the knee joint.
Finger Tendon Glides: Start with fingers straight, then curl them into a hook, then a full fist, then a straight fist. Return to start. 10 reps. Essential for hand and finger arthritis — maintains tendon mobility.
Hip Abduction (Side-Lying): Lie on your side, legs stacked. Lift the top leg 18–20 inches, hold 2 seconds, lower slowly. 10–12 reps each side. Strengthens hip stabilisers critical for knee and hip OA.
Shoulder Pendulum Swings: Lean forward, supporting yourself on a table with one hand. Let the other arm hang loose and gently swing in small circles. 30 seconds each direction. Relieves shoulder joint compression.
Standing Heel Raises: Hold a wall for balance. Rise onto your toes slowly, lower slowly. 15 reps. Builds calf strength, supports ankle stability, and stimulates cartilage health through gentle loading.
Living Well Beyond the Clinic: Lifestyle Strategies
Physiotherapy is most powerful when it becomes part of a broader lifestyle approach to arthritis management. Your physiotherapist will likely reinforce several evidence-based habits:
Pacing & Activity Management: Learning to balance activity with rest — avoiding both sedentary stretches and overexertion — is a skill that physiotherapists actively teach. Boom-and-bust cycles are one of the leading causes of flares.
Heat & Cold Therapy: Heat relaxes muscles and reduces morning stiffness; cold reduces acute inflammation after activity. Your physio will guide you on when and how to apply each for your specific joints.
Weight Management: Each kilogram of excess body weight places approximately 4 kg of additional force on your knee joints. Even modest weight loss in combination with physiotherapy produces dramatic symptom improvements for lower limb arthritis.
Sleep Hygiene: Poor sleep amplifies pain perception. A physio can advise on joint-protective sleeping positions and supports (pillows, bed wedges) that dramatically improve sleep quality for arthritis patients.
Consistency beats intensity. Fifteen minutes of gentle movement every day will always outperform an intense hour-long session once a week. Build small, sustainable habits — your joints will thank you over months and years, not just days.
When to Seek Help: Signs It's Time to See a Physiotherapist
You don't need to be severely debilitated to benefit from physiotherapy. Seek a referral if you're experiencing: joint pain lasting more than 6 weeks; morning stiffness for longer than 30 minutes; difficulty with everyday tasks like climbing stairs, opening jars, or walking comfortable distances; or if you've had a recent arthritis diagnosis and aren't sure where to start.
Early intervention is always more effective. Waiting until pain is severe or function is significantly impaired makes recovery longer and harder.